You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
It is said that patients do not care what you know, until they know that you care.
The team approach centers around the synergy between the skills inherent in both the restorative and surgical offices. However, this synergy is about much more than just the technical skills, it is about the value of a multi-office approach to patient management. When each treating office develops a plan focusing on the patient’s best interest, patient understanding and trust follow naturally.
The greatest value of this team effort becomes apparent while dealing with the more challenging cases involving defects of bone, soft tissue, and dentition that are extensive enough to reduce the probability of a complete natural reconstruction. Educating patients about the limitations of their individual case during the treatment-planning phase facilitates acceptance and appreciation of the proposed treatment. A successful team approach occurs when two separate entities can each clearly delineate the treatment challenge, describe their portion of the ideal plan to manage it, and accurately describe the expected outcome.
Perspectives on Treatment-Planning
It has long been accepted that the surgeon’s understanding of the restorative challenge is essential to creating the best possible treatment plan. The realization that it is the restoration, not the residual bone, that should define implant placement led to natural implant-based reconstruction. When referring a patient to a surgeon for evaluation, it is important that the restorative office be clear about its reasons for the referral and any restorative issues that can be anticipated. When the restorative office is either unsure about what is possible or fails to provide relevant information, the surgical office is in the difficult position of needing to plan treatment when the restorative challenges have not been identified, especially to the patient. When cases are attempted under these circumstances, unanticipated problems can hinder achievement of the desired result and often produce a less-than-satisfied patient.
When examining the state of modern implant reconstruction, it is apparent that treatment planning may be more effective when the restorative office also has an understanding of the surgical potential. Without a practical understanding of surgical options, patients may not receive the most appropriate referral from their restorative office. For example, a restorative practice may not realize that surgical implant placement can be atraumatic and that it may be the easiest possible treatment for the patient. Without this understanding, the aggressive preparation of adjacent non-restored teeth may seem reasonable. In addition, assumptions about cost may inhibit a referral, although studies have demonstrated that when patients are educated about value, their willingness to invest in their oral health increases. If the restorative office does not understand the minimum space requirements for treatment, communication with or inclusion of an additional team member, such as an orthodontic specialist, may not occur before the patient’s treatment is finalized. Not realizing the value of maintaining an adjacent tooth, the restorative office may not utilize an endodontic specialist.
Identifying the challenges to treatment does not impede case acceptance, if the patient feels those concerns are being well managed. Referral to a surgical specialist who reviews the concerns identified by the restorative dentist, explains how they will be managed, and describes how the restorative dentist is planning to manage residual issues may lead to higher case acceptance rates.
To facilitate a treatment consultation for a single missing anterior tooth, the patient should be educated about the assumption that every missing tooth has lost some soft tissue and bone. Working through the magnitude of the reconstruction required, the clinician could begin by inquiring what the patient wants at that moment, without regard to cost, and imagining the treatment without involving a drill or anesthesia. To help identify the important issues, focusing questions are useful: What do you like best and least about your smile? What would you change?
Managing All Aspects
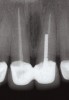
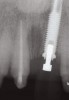
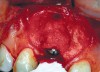
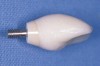
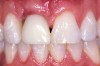
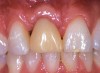
Communicating the desired restoration to the surgeon is done effectively through the creation of an accurate, well-fitting surgical guide, which is used with radiologic markers in a cone beam scan or conventional radiographs. The desired emergence profile clearly marked on the surgical guide indicates for the surgeon the magnitude of any possible osseous and soft-tissue reconstruction. It also may prompt a discussion of the surgical limitations of a case, as it may not be possible to completely restore the lost soft tissue and bone (Figure 1 and Figure 2).
Treatment planning begins with a relative understanding of the force that will be applied to the area in question. In the esthetic zone, the goal is to plan for the narrowest implant that will effectively manage the expected load. As an implant gains diameter, it becomes significantly stronger; at the same time, a larger implant results in less biologically active material (bone), which is necessary for natural soft tissue.
Next, how the native bone that surrounds the missing tooth impacts the soft tissue should be considered. The height of the soft tissue papillae on each side of the proposed single-tooth implant is directly related to the amount of bone on the adjacent natural teeth. The seminal work of Dennis Tarnow, DDS,1-4 and John Kois, DMD, MSD,5 has demonstrated that if the bone present on the natural teeth adjacent to the edentulous area can be maintained, it can be predicted that there will be a soft-tissue papilla of 4 mm from this interdental bone. It is also necessary to recognize that the vertical height of interdental alveolar bone on the adjacent natural teeth cannot be surgically increased predictably, which may produce a final result with a deficient soft-tissue papilla. Restoratively, if the interproximal papilla is expected to be deficient and this is a concern to the patient, the treatment plan should include redoing or initiating a crown or veneer on the adjacent tooth. This restoration, along with the implant restoration, will allow the obturation of the deficiency in the most symmetrical and esthetic manner possible.
The bone on the adjacent natural teeth is extremely valuable; it is necessary to leave enough space from the body of the implant to the adjacent teeth to avoid impacting the vitality of this bone. Some recent studies suggest 3 mm or more of space may be optimal; certainly an implant less than 1 mm from the natural tooth will often result in damaging bone loss. The goal is to plan for a 2-mm space from the body of the smallest implant that will manage the potential load to the adjacent natural tooth.
The potential emergence profile is directly related to the vertical position of the head of the implant. As implant options have expanded, there is variability in how much bone can be maintained around the head of an implant, which directly impacts the amount of soft tissue and the resulting emergence profile. A good baseline is a traditional hex-top implant. It is expected that with good surgical placement of the labial edge of the implant approximately 2 mm lingual to the desired emergence profile, an emergence of about 2.5 mm from the head of the implant can be attained.6-9 This example assumes a minor amount of bone remodeling or loss around the head of the implant, but nevertheless results in excellent predictability for the future emergence of the final crown. Maintaining more bone with a newer-generation implant (such as an internal conical connection implant with abutment diameter reduction) can require sinking the implant more apically when there is excess bone to achieve the same desired emergence.
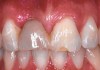
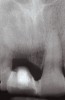
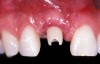
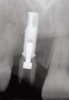
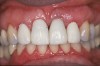
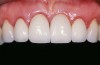
An example of effective patient treatment management (Figure 3 through Figure 11) demonstrates the synergy desired in patient treatment. In this case the surgeon effectively manages the implant placement along with the bone and soft-tissue grafts to idealize implant position and the soft-tissue frame to the potential restoration. The surgical treatment is followed with the restorative dentist managing and guiding the soft-tissue redevelopment with a carefully developed provisional restoration and, finally, the placement of a final restoration that mimics the patient’s own natural dentition.
Communicating the Challenges
If during consultation with the surgeon, the team recognizes that the implant placement—whether due to a lack of bone that can be grafted or patient-induced limitations—will lead to a less-than-ideal result, this information is invaluable for the preoperative patient consultation. The patient may not be concerned that the future replacement tooth may have an emergence more apical than the adjacent natural teeth, but it is better to have this discussion before the treatment begins. If the patient expresses dissatisfaction with a probable asymmetric outcome, and if the future implant position cannot be improved, further discussion about crown lengthening on adjacent teeth or perhaps additional restorative possibilities may be necessary.
One often-overlooked area of restorative patient management is the effective use of provisionals. Patients may interpret a 3- to 6-month healing phase as a period when they will be unable to live a normal life. It is, therefore, very important to communicate to patients that a single or series of provisionals will maintain their quality of life, and sometimes even improve it. For an advanced case, two or more different or altered provisionals may be necessary to carry the patient through to the final restoration. The cost of these provisionals may be substantial, and therefore should be included in the initial patient presentation. The restorative dentist also needs to plan for the costs of removing and rebonding a bonded provisional. On some challenging cases—eg, those that require substantial bone and/or soft-tissue grafting—it may be very difficult to make a provisional that does not negatively impact the healing site. As the surgical site will swell during the first 24 hours, placing a rigid temporary that impinges on the tissue during this healing period ultimately may result in less tissue. Poorly made treatment partials can put pressure on the soft tissue and bone and even mobilize an implant if the transmission of force is not controlled. Once the implant can be loaded directly, the considerations for using a provisional or proceeding to the final restoration should be evaluated. If the final restoration will include a custom abutment, developing the final gingival shape before committing to a specific cement margin position may be especially critical. It has been documented that the gingival tissue continues to reorganize over a 6-month period.10 To attain the ideal margin position, it is advantageous to use a provisional during this healing period. The restorative dentist should undercontour the provisional or the abutment subgingivally, especially on the labial, to maximize the thickness and vertical height of the gingival (Figure 12 and Figure 13).
The creation of the final restoration should be an accurate reflection of the original plan. Options include a screw access hole to the lingual, allowing for a screw-retained restoration if desired, or through the incisal or labial third of the final restoration, most often resulting in a custom abutment and cemented crown. The effective use of a zirconium custom abutment and cemented all-ceramic crown can lead to superior esthetic results when the cement margin has been created in the correct position, which is less than 1 mm subgingivally. However, with crown cementation on abutments, it is extremely easy to leave residual cement. Left apical to the margin, residual cement may cause catastrophic soft-tissue and bone inflammation and loss.
Conclusion
If the patient has been well informed, any specific limitation has already been discussed and accepted before the final restoration is inserted. This can occur only when both the surgeon and restorative dentist have a strong understanding of the expected result based on biologic expectations of bone, soft tissue, and implant position. When appropriate, adjunct procedures should be planned for and initiated to overcome esthetic issues (Figure 14) before the final restoration is inserted. When the surgical office understands the restorative challenges and the restorative office understands the surgical challenges, the most effective treatment plans are developed. Communicating these challenges to patients early in the treatment planning cycle prepares them for the uniqueness of their situation and guides them to consider additional procedures to obtain optimal results. Most often, a single office does not develop the exceptional skill sets needed to manage a complex rehabilitation, both surgically and restoratively. By coordinating two offices—each managing different parts of the treatment, but demonstrating cohesiveness and mutual respect—the highest level of patient satisfaction and acceptance is achieved.
About the Author
George R. Perri, DDS
Private Practice
Whittier, California
Lecturer in Advanced Prosthodontics
UCLA School of Dentistry
Los Angeles, California
References
1. Tarnow DP, Eskow RN, Zamzok J. Aesthetics and implant dentistry. Periodontol 2000. 1996;11:85-94.
2. Tarnow DP, Eskow RN. Preservation of implant esthetics: soft tissue and restorative considerations. J Esthet Dent. 1996;8(1):12-19.
3. Tarnow DP, Eskow RN. Considerations for single-unit esthetic implant restorations. Compend Contin Educ Dent. 1995;16(8):778-784.
4. Tarnow D. Esthetic excellence with the single-tooth implant. Dent Econ. 1993;83(3):80-82.
5. Kois JC. Predictable single-tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11):895-900.
6. Jovanovic SA . Esthetic therapy with standard and scalloped implant designs: the five biologic elements for success. J Calif Dent Assoc. 2005;33(11):873-880.
7. Paul SJ, Jovanovic SA. Anterior implant-supported reconstructions: a prosthetic challenge. Pract Periodontics Aesthet Dent. 1999;11(5):585-590.
8. Torreão AS, Fonseca DM, Jovanovic SA . Single-unit implant-supported restoration in the vertically deficient anterior maxilla. Pract Periodontics Aesthet Dent. 1999;11(5):571-575.
9. Jovanovic SA , Paul SJ, Nishimura RD. Anterior implant-supported reconstructions: a surgical challenge. Pract Periodontics Aesthet Dent. 1999;11(5):551-558.
10. Bengazi F, Wennström JL, Lekholm U. Recession of the soft tissue margin at oral implants. A 2-year longitudinal prospective study. Clin Oral Implants Res. 1996;7(4):303-310.